Medscape National Physician Burnout & Suicide Report 2021

Feeling stressed or even burnt-out? You’re not alone. As the COVID-19 pandemic continues to rage, we all continue to struggle mentally as we feel we don’t have control over our lives and work, are under chronic levels of stress and unsustainable workloads. According to a new HBR survey of nearly 1,500 people from 46 countries, 86% of us reported a decline in general and workplace well-being.
So, yes, physician burnout is severe today, but the seeds were planted before Covid-19 hit — even then, many workers were already experiencing high levels of it. The pandemic was simply an accelerant.
In healthcare, the picture is bleaker because the industry was struggling with stress and burnout even before COVID, mostly due to increase in bureaucratic tasks and a sense of loss of control. Many physicians and nurses are affected by this state due to work overload and feelings of helplessness. However, burnout has been amplified by the pandemic and the surge in the cases that physicians have to handle every day.
In early 2020, physicians, nurses, and first responders were celebrated as heroes with parades and daily applause. Over time the cheers stopped. The applause faded at the worst possible time — when health care workers needed it most. They already had the highest rates of burnout, but the pandemic took them to unprecedented levels.
In the recent 2021 Medscape survey: 12,000 physicians from various specialties shared what they struggled with during the pandemic. Here are 5 key takeaways from the survey and our suggested strategies to address the next pandemic in healthcare.
5 Key Takeaways About Physician Burnout
1 – Critical Care is the Most Burnout Specialty
Across all specialties, 42% of the physicians reported burnout, with the highest rates being among Critical Care, Rheumatology, Infection Disease, Pulmonary Medicine, Neurology, Family and Internal Medicine.

Burnout by Speciality Source: Medscape Burnout Survey 2021
2 – Thirteen percent (13% ) of Physicians Thought of Suicide while 1% attempted it
It is sad that we lose one physician per day to suicide. In 2018, 300 physicians committed suicide, that is double any other profession. The more frighting survey result is that 1% of the physicians attempted suicide. There is no other profession more worthy of our empathy and coaching.

Source: Medscape 2021 Survey
3 – Women Physicians Experience More Burnout than Men
Over the years, women reported more burnout than their male counterparts as they tend to assume more responsibilities at home and work. This year, the pressure has increased due to kids being homeschooled, and the fears of bringing the virus home in addition to everything else they had to deal with before the pandemic.
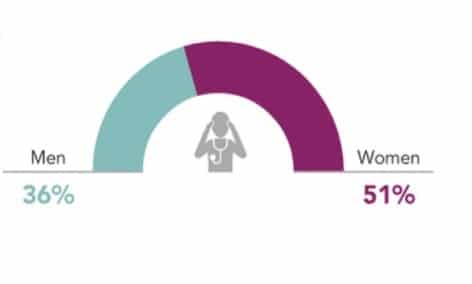
Burnout by Gender Source: Medscape Burnout Survey 2021
4. Burnout Started way Before COVID-19
We have been reporting (check out our previous posts here) that stress and exhaustion leading to physician burnout and burnout for medical providers have been in existence within the medical community way before COVID and advocating for making clinician experience as important as patient experience. In the Medscape 2021 Survey, 79% of the physicians surveyed confirmed that burnout started way before COVID while 21% reported that they experienced stress and exhaustion after COVID due to many factors including lack of PPE, watching their patients die without their families, and chronic stressful conditions due to COVID cases.
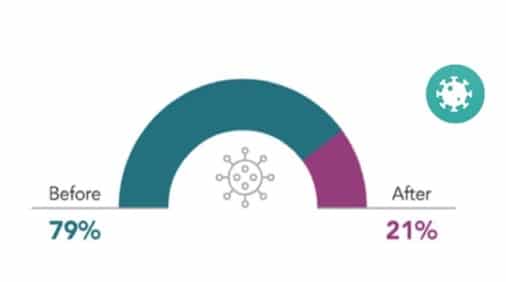
Burnout before and after COVID Source: Medscape Burnout Survey 2021
5 – Bureaucratic Tasks are still 58% of Causes of Burnout
In 2016 Medscape, too many bureaucratic tasks and spending too many hours at work were the top 2 causes of burnout. Unfortunately, in 2021 these factors have not changed.
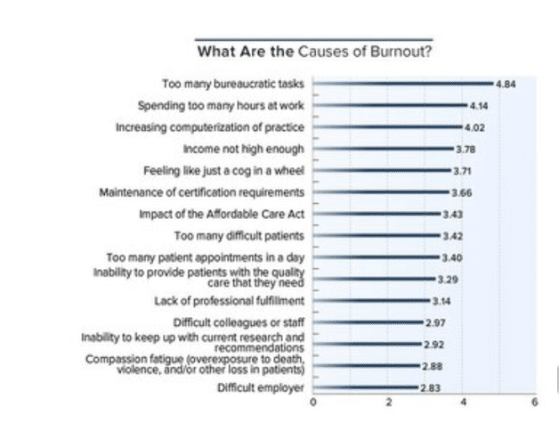
2016 causes of burnout Source: Medscape Burnout Survey 2016
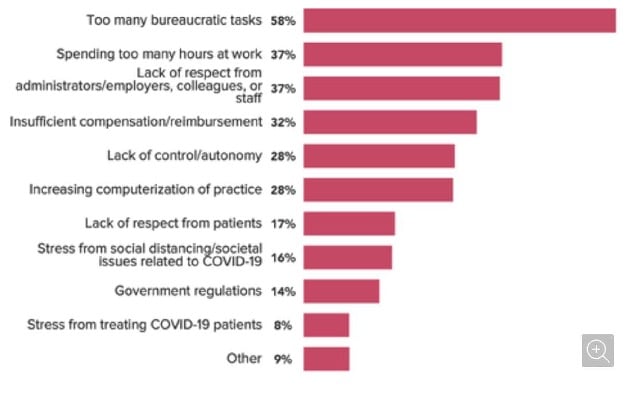
2021 causes of Burnout (Still the same as 2016) Source: Medscape Burnout Survey 2021
How to Help Solve Physician Burnout
Albert Einstein once said: “the definition of insanity is to continue to do the same things and expect a different outcome.”
I have great concerns that we still prescribe self-care as the cure for burnout. We’ve put the burden of solving the problem squarely on the shoulders of the clinicians. Recommendations for more yoga, mindfulness, meditation, and exercise are typically what the response has been. But those are tools for improving well-being and not preventing burnout. What is needed are upstream strategies that address the roots of the causes, not downstream tactics that address only the symptoms.
Focus on Clinician Experience as Being Equal to Patient Experience
While the focus by organizations and leaders has been on patient experience, we all know that you can’t give what you don’t have. Clinicians can’t achieve a high level of patient satisfaction when they are running out of capacity, lack work life balance and are stressed, depressed and suffering from burnout.
Shift the formula: Patient Experience = Clinician Experience – Hassle Factors
Assess and Address the Hassle Factor Index
Using a hassle factor index survey (free copy can be found here on the HLI website) to help your nurses and physicians identify the hassle factors that are in their way causing them stress, frustration and extra work. For example, during the pandemic, the lack of available PPE was a key hassle factor. Before the pandemic, the number 1 hassle factor was documentation in the Electronic Medical Record and bureaucratic tasks.
Virtual Assistants
The best solution to help reduce the bureaucratic tasks and spending many hours at work (the top 2 causes of burnout in the survey), is to hire a virtual assistant to take care of all documentation and bureaucratic task so physicians can spend more time at home. For a small fee/day, you can have a virtual assistant full time working for you. Link to free trial.
Coaching
There is more evidence than ever that professional healthcare coaching helps reduce burnout. In the JAMA Internal Medicine, Research conducted at the Mayo Clinic showed that professional coaching of physicians is a potentially effective intervention to improve physician well-being. The authors report that physicians who completed six private sessions with a professional coach showed significant decreases in emotional exhaustion and overall burnout, in addition to increases in quality of life and resilience. These results offer hope for physicians.
From our own experience at HLI, coaching physicians and nurses has reduced the level of stress and mental strains. For free coaching consultation, contact us online.
Reduce workload/Create Not to Do list
Let’s stop the madness! Let’s stop saying “do more with less” and start doing less. During these stressful times, less is more. This is the time to develop a “NOT TO DO LIST” by challenging the need for many projects, many metrics, many meetings and due dates. (See article on Creating Not to Do list)
Invest and Improve Frontline Clinical Leadership
Empathetic Leadership is now more critical than ever. We need clinical leaders that would empathize with their stressed-out team members. Being empathetic starts with the leader acknowledging that things are not the same as before, listening well to their team members and taking actions to address hassle factors or sometimes just simply listening without the need to take any actions. Leaders need to create a psychological safety for people to say I am not ok. Leadership is crucial during times of crisis. We have had the privilege to be on coaching calls with healthcare leaders and physicians during times of crisis and are always humbled by their compassion and dedication. Download a complimentary CTI whitepaper in which we identify the 3 most important tools leaders can use during a crisis and provide guidance on how best to apply them with your team.
Provide Wellbeing Resources to Your Clinicians
Here are some free resources that you can share with your clinicians:
- Burnout Assessment – HLI provides a free burnout assessment tool that can help you determine if you are headed down the burnout path. Upon completing the survey, you will receive a score that will help you determine where you fall on the burnout spectrum.
- Resources to restore personal Energy: During a prolonged crisis, it feels like everything desirable is in short supply. That is especially true when it comes to the resources we rely on to restore our personal energy. Our best option, in this case, is to focus on maximizing the opportunities that we have easily made available for personal restoration in times of prolonged energy drain. Here are 2 vital steps for restoring your energy during a crisis.
- Webinar on Resilience under Pressure: A free webinar is offered by HLI on resilience under pressure. Challenging times can easily make us feel as though we have no control over our commitments to care for others and no time to care for ourselves. This webinar includes some viable practices for physicians to restore their energy in the midst of a busy schedule, with little intrusion and big benefits.
- The Harvard Business Review recently published an article on the main causes of burnout, how we got to this point, providing additional suggestions on how to beat burnout.
Given we all entrust our family’s health and lives to our physicians all the time, let’s do everything we can to support those physicians and to take care of them first, so they can take good care of our families and loved ones when we need them.
A sincere gratitude to all our healthcare frontline heroes. We feel your pain and we are here to help!!
Contact us for more information on coaching, resilience and well-being services for you or your team.
References:
HBR. Beyond Burned Out by Jennifer Moss
Dyrbye, Shanfelt, Gill, Satele, West. (2019) Effect of a Professional Coaching Intervention on the Well-being and Distress of Physicians. A Pilot Randomized Clinical Trial. JAMA Internal Medicine.







